ABSTRACT Introduction: The majority of the published literature on contemporary military medicine contradicts the concept of austere. Operational medicine is part of every armed conflict around the world, while armed forces of most countries internationally have limited medical resources especially in the front line. The aim of this review is to identify the particularities of a truly austere environment and present a short guide of preparation and action for military medical personnel internationally. Materials and Methods: An exhaustive search of the existing English literature on operational and military medicine in austere environments was carried out in EMBASE and PubMed databases. Results: This review included seminal and contemporary papers on the subject and synthesized a multiperspective short guide for operational medical personnel. Discussion: Experience from forward surgical teams of the U.S. Army and humanitarian teams of physicians in war zones who work under precarious and austere circumstances has shown that the management of casualties requires different strategies than in higher levels of combat casualty care and in a civilian setting. A number of factors that must be controlled can be categorized into human, environmental, equipment-related, and socioeconomic. Surgeons and other medical personnel should have knowledge of these aspects beforehand and be adequately trained in peacetime. Physicians must master a number of essential skills and drugs, and be familiar with dosage regimens and side effects. Conclusion: The military surgeon must be specially trained and prepared to use a wide range of skills in truly austere environments in contemporary conflicts.
https://academic.oup.com/milmed/advance-article/doi/10.1093/milmed/usz467/5716503
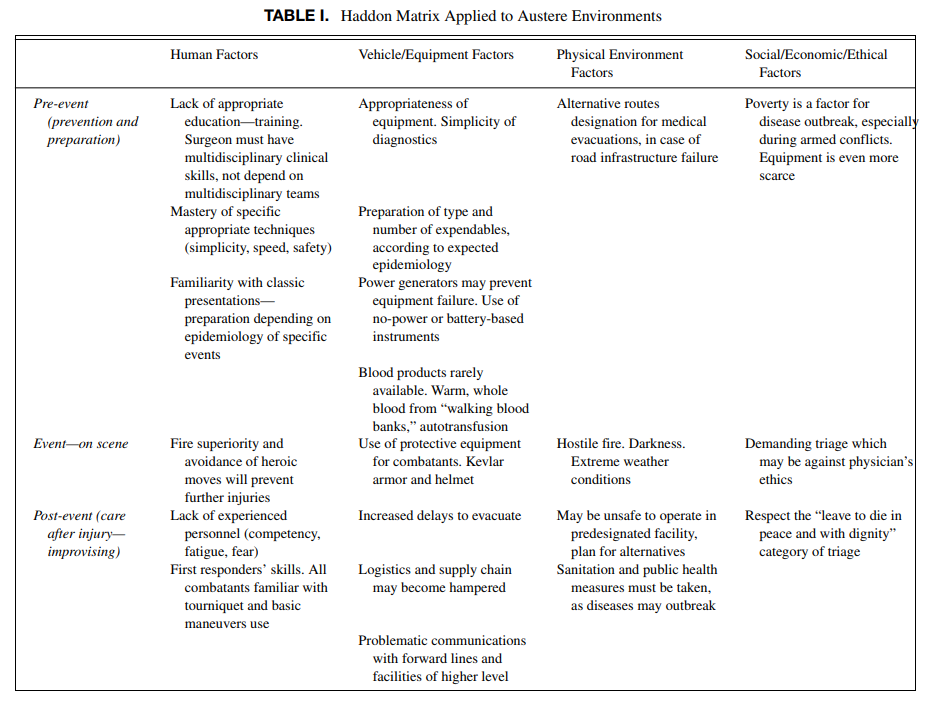
This article outlines four factors that affect the practice of medicine in austere environments.
- Human factors
- Medical, Mobility, and Protective Equipment factors
- Physical Environment factors
- Social, Economic, and Ethical factors
Key Points
Much can be done to prepare before a crisis occurs. Education and training, selection of equipment, and operational planning all play a role in increasing provider effectiveness “on the X”.
As a Prussian General once said “no plan survives contact with the enemy”. Medical planners must develop alternative and contingency plans to compensate for the ever-changing nature of austere environments or the tactical considerations of the military environment.
Multidisciplinary competence is the linchpin of successful austere medicine for both medical and non-medical personnel. Reliance on high-dollar equipment, robust logistics trains, and rapid access to both the former, is an artifact of wars waged by the most well-funded armies the developed nations can field. True austerity, whether through socioeconomic factors or from large-scale combat operations with near-peer opponents will create challenges to which we are not accustomed.
Offering medical assistance under precarious circumstances is a demanding, multidimensional task that requires good preparation and sharp thinking and acting. There is no panacea recipe to be followed during these situations. However, many of the principles are core capacities and the doctor is then expected to adjust and improvise in the unique environment.
Needs should be fitted to epidemiology, and alternatives for equipment and infrastructure should be preplanned. Appropriate training with the necessary equipment in the predeployment period is of the outmost importance for the maintenance of the essential skills and readiness, which improves the outcomes of the injured and sick in the field.